Page Contents
Foot care is often overlooked in older adults, yet it plays a central role in mobility, independence, and overall quality of life. As people age, physiological changes such as reduced skin elasticity, diminished circulation, and altered biomechanics increase vulnerability to foot problems. Even minor issues, when neglected, may progress into significant complications that affect gait, balance, and the ability to perform daily activities. In geriatric practice, maintaining foot health is not simply about comfort; it is a key component of preserving function and preventing disability.
Prevalence of foot conditions in the elderly
Foot disorders are highly prevalent among older populations. Studies indicate that up to 70 to 80 percent of elderly individuals experience at least one foot problem, ranging from mild nail disorders to severe deformities. In institutional settings such as nursing homes, prevalence rates are often higher due to comorbidities, reduced mobility, and dependency on caregivers for personal hygiene. Chronic conditions such as diabetes and peripheral vascular disease further increase the risk, making foot problems a routine yet serious concern in geriatric care.
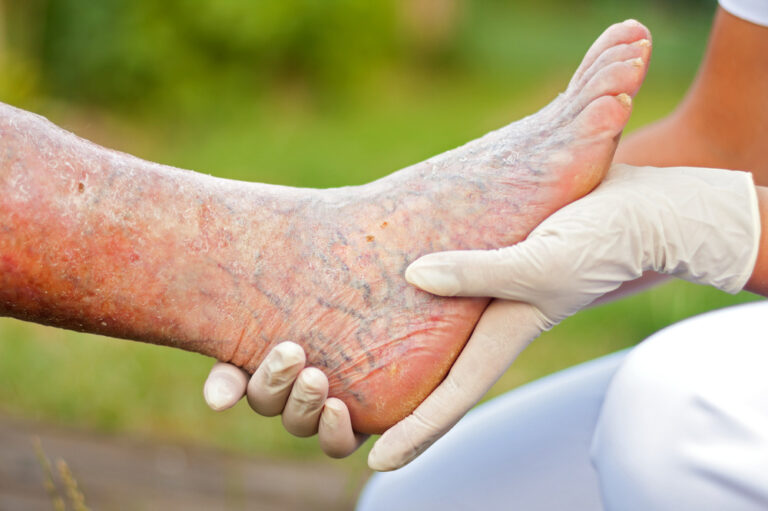
Common foot conditions in the elderly
Older adults frequently present with a range of foot conditions. These conditions often coexist, compounding their impact on mobility and pain levels. These include:
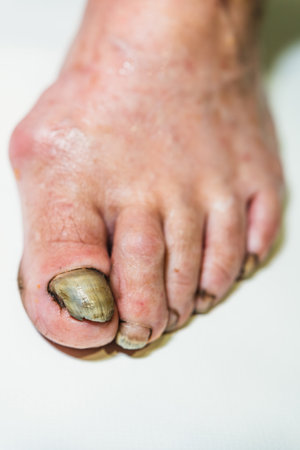
- Nail disorders, such as onychomycosis and thickened nails, which may cause discomfort and difficulty in walking
- Calluses and corns, resulting from prolonged pressure and friction
- Foot deformities, including bunions, hammer toes, and claw toes, often linked to long-term biomechanical stress
- Skin conditions, such as dryness, fissures, and infections
- Ulcers, particularly in individuals with diabetes or poor circulation
- Heel pain and plantar fasciitis, associated with changes in foot structure and fat pad atrophy
Root causes of foot conditions
The development of foot problems in older adults is multifactorial.
- Age-related changes in skin and soft tissues lead to thinning, reduced resilience, and slower healing.
- Circulatory decline reduces oxygen and nutrient supply to tissues, increasing susceptibility to injury and infection.
- Neurological conditions, including peripheral neuropathy, impair sensation, which delays recognition of injury.
- Poorly fitting footwear remains a major contributor, especially when combined with deformities.
- Chronic diseases such as diabetes, arthritis, and obesity place further stress on the feet, accelerating deterioration.
Implications of delayed treatment
Delayed management of foot conditions may lead to serious complications. Minor lesions can progress to infections, particularly in individuals with compromised immunity or diabetes. Untreated ulcers may deepen, increasing the risk of osteomyelitis and, in severe cases, amputation. Pain and deformities alter gait patterns, leading to instability and increased risk of falls, which are a major cause of morbidity in the elderly. Reduced mobility may then contribute to muscle deconditioning, social isolation, decline in overall health status and quality of life.

Treatment options
Management of foot conditions in older adults requires a comprehensive and individualised approach. Early intervention often leads to better outcomes and prevents progression to more severe complications. Common interventions include:
- Routine podiatric care, including nail trimming, callus debridement, and skin care
- Footwear modification, ensuring proper fit, cushioning, and support
- Orthotic devices, to redistribute pressure and correct biomechanical issues
- Topical and oral medications, for fungal infections or inflammatory conditions
- Wound care management, particularly for ulcers, involving dressings, offloading, and infection control
- Multidisciplinary management, involving physicians, nurses, and physiotherapists for complex cases
Prevention of foot conditions
Preventive strategies are essential in geriatric foot care. Preventive care should be integrated into routine health assessments in both community and institutional settings. Key measures include:
- Daily inspection of the feet, especially for those with reduced sensation
- Regular washing and thorough drying, particularly between the toes
- Use of moisturisers to prevent skin dryness and cracking
- Wearing well-fitted, supportive footwear at all times
- Routine podiatry reviews, especially for high-risk individuals such as those with diabetes
- Education of caregivers on proper foot hygiene and early signs of problems
Conclusion
Foot health in older adults requires consistent attention and proactive management. Regular screening allows early identification of problems before they escalate into serious complications. Prevention remains the most effective strategy, supported by routine care, appropriate footwear, and timely professional intervention. In geriatric practice, prioritising foot care contributes directly to maintaining mobility, reducing fall risk, and preserving independence.
