Page Contents
Kidneys filter waste, excess fluid, and toxins from blood. Kidney failure occurs when this filtration function drops to a low level. Doctors call this end stage kidney disease.
Patients with severe kidney failure develop fluid overload, electrolyte imbalance, and toxin accumulation. Symptoms include fatigue, breathlessness, nausea, confusion, swelling of legs, and reduced urine output.
Dialysis replaces part of the kidney’s filtering role. Blood passes through a filter which removes waste and extra fluid. Without dialysis or kidney transplant, advanced kidney failure leads to progressive deterioration and death.
Prevalence of elderly people who require dialysis
Ageing populations drive a steady rise in kidney failure. Chronic diseases such as diabetes and hypertension damage kidneys over many years. Globally, more than 3 million patients receive dialysis treatment. A large proportion fall within the elderly group.
In Singapore, chronic kidney disease affects about 1 in 10 adults. Diabetes remains the leading cause. Elderly patients above 65 years represent a growing proportion of new dialysis cases.
Several factors explain this trend.
- Longer life expectancy
- High prevalence of diabetes and hypertension
- Better detection of chronic kidney disease
- Wider access to dialysis services
As life expectancy rises, clinicians and families face difficult decisions on dialysis for frail elderly patients.
Why dialysis is needed? How dialysis works?
Healthy kidneys perform three key functions.
- Remove metabolic waste from blood
- Regulate electrolytes such as potassium and sodium
- Maintain fluid balance
When kidney function drops below about 10 to 15 percent, the body struggles to maintain these processes.
Dialysis works by filtering blood through a semi permeable membrane. Two main processes occur.
- Diffusion. Waste substances move from blood into dialysis fluid
- Ultrafiltration. Extra fluid moves across the membrane through pressure difference
Note: Dialysis does not cure kidney disease. It only replaces part of kidney function and usually continues for life unless a transplant occurs.
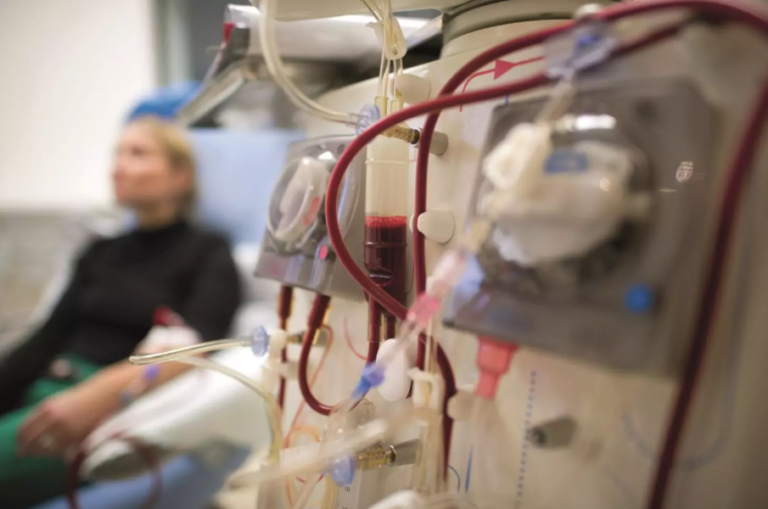
Different types of dialysis
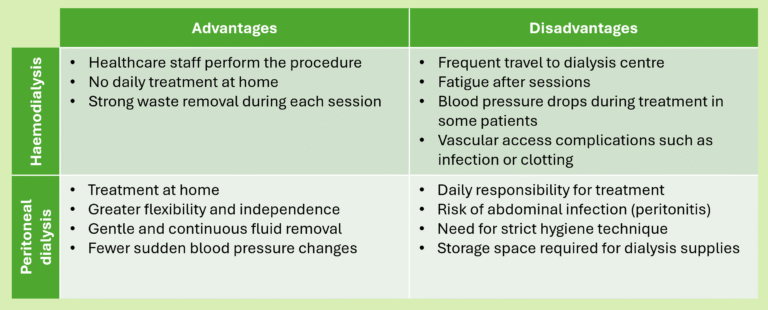
There are two main dialysis methods.
Haemodialysis
Haemodialysis filters blood through a machine called a dialyzer. Blood leaves the body through a vascular access, passes through the machine, and returns after filtration.
Peritoneal dialysis
Peritoneal dialysis uses the patient’s abdominal lining as the filtration membrane. A soft catheter enters the abdomen. Dialysis fluid fills the abdominal cavity and absorbs waste and excess fluid. After several hours, the fluid drains and fresh fluid replaces it.
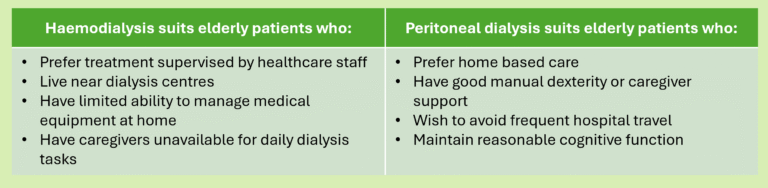
Which dialysis suits elderly patients?
The best dialysis method depends on medical condition, functional ability, and social support. Many elderly patients face mobility limitation, cognitive decline, and multiple chronic diseases. These factors influence dialysis choice.
Cost considerations also influence decision. Peritoneal dialysis often costs less due to fewer facility charges. Actual out of pocket expenses vary widely after subsidy. Clinical studies show survival rates between the two methods remain broadly similar in many elderly patients during the first few years of treatment. Quality of life, independence, and caregiver burden often shape final decisions.
Tips for protecting kidney health
Kidney disease develops slowly over many years. Early lifestyle choices influence long term kidney health.
You protect kidneys through the following steps.
- Control blood sugar if living with diabetes
- Monitor blood pressure regularly
- Maintain healthy body weight
- Reduce salt intake
- Avoid smoking
- Exercise regularly
- Drink adequate water
- Avoid excessive use of painkillers such as non steroidal anti inflammatory drugs
- Attend regular health screening
Conclusion
Dialysis replaces an essential life sustaining function when kidneys fail. Haemodialysis and peritoneal dialysis both serve this purpose through different approaches.
For elderly patients, the decision rarely depends on medical factors alone. Functional ability, caregiver support, lifestyle preference, and cost play equally important roles.
The most suitable dialysis option aligns with the patient’s health status and personal priorities. Clear discussion with healthcare professionals helps patients and families make an informed and realistic choice.
