Page Contents
Low platelet count is called thrombocytopenia. Platelets help stop bleeding by forming clots at injury sites. When levels fall, the body loses part of this protective function. Most elderly patients find out through routine blood tests during chronic disease follow up, medication monitoring, or hospital admission. In nursing homes, periodic screening often detects the issue before symptoms appear.
A normal platelet count ranges from about 150,000 to 450,000 per microliter of blood. Thrombocytopenia is defined as a count below 150,000.
- Mild: 100,000 to 150,000
- Moderate: 50,000 to 100,000
- Severe: below 50,000
- High risk of spontaneous bleeding: below 20,000
Prevalence in elderly population
Thrombocytopenia is common in older adults, especially in hospital and long term care settings. The prevalence rises with age due to chronic illness, polypharmacy, and bone marrow disorders. In acute care, many elderly patients develop low platelet counts during admission, often linked to infection or treatment effects. In nursing homes, mild thrombocytopenia is often stable and monitored over time. Ageing itself does not directly reduce platelet count. The pattern reflects accumulated disease burden.

Common causes in elderly
Causes fall into three main mechanisms. Reduced production, increased destruction, and sequestration.
- Reduced production occurs when the bone marrow fails to produce enough platelets. This is seen in conditions such as myelodysplastic syndromes, leukemia, nutritional deficiencies, and the effects of chemotherapy or chronic alcohol use.
- Increased destruction happens when platelets are produced but removed too quickly from circulation. Immune thrombocytopenia, drug induced reactions, severe infections, and autoimmune diseases are key contributors in elderly patients.
- Sequestration refers to platelets being trapped in an enlarged spleen. This is often linked to chronic liver disease and portal hypertension.
In practice, more than one mechanism often exists. For example, an elderly patient with infection who is also on multiple medications may develop combined causes.
Clinical implications
Many patients with mild thrombocytopenia remain asymptomatic. The condition is often detected incidentally. As platelet levels fall, bleeding risk becomes more evident.
- Easy bruising with minimal trauma
- Petechiae on the skin
- Prolonged bleeding from minor cuts
- Gum bleeding or nosebleeds
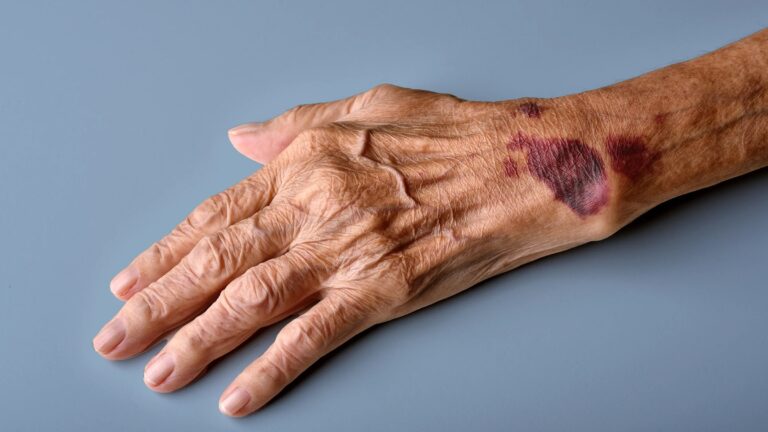
Severe thrombocytopenia can lead to life threatening complications such as gastrointestinal bleeding or intracranial hemorrhage. In frail elderly, even minor bleeding can trigger functional decline. A simple fall may result in major bleeding due to reduced clotting ability.
Treatments available
Management depends on both cause and severity. Mild and stable cases often require observation with regular monitoring. Reversible causes such as nutritional deficiency should be corrected early.
Drug related thrombocytopenia requires prompt identification and withdrawal of the offending agent. Platelet levels often recover once the drug is stopped.
Immune related cases require targeted therapy to reduce platelet destruction.
- Corticosteroids to suppress immune response
- Intravenous immunoglobulin for rapid platelet increase
- Second line agents for resistant cases
Severe thrombocytopenia or active bleeding requires urgent care. Platelet transfusion and hospital management are often necessary. Bone marrow disorders require specialist input and disease specific treatment.
Side effects of medications
Treatment risks are higher in older adults due to comorbidities and multiple medications. Close monitoring is required. Use the lowest effective dose and monitor closely to reduce complications.
- Corticosteroids are effective but commonly raise blood sugar and increase infection risk. They also cause fluid retention, muscle weakness, and mood changes, which raise fall risk.
- Intravenous immunoglobulin works quickly but may lead to fluid overload and headaches. Frail patients with heart disease face higher risk. Rarely, thrombosis can occur.
- Platelet transfusion gives short term benefit. Risks include transfusion reactions and fluid overload. Repeated use may reduce effectiveness.
- Stopping a causative drug must be done carefully. Sudden withdrawal may worsen underlying conditions such as stroke risk or seizures.
Does lifestyle modification help?
Lifestyle changes support safety rather than directly correcting platelet levels. The focus is on reducing bleeding risk and maintaining overall health.
- Prevent falls through safe environment and supervision
- Use gentle oral care to avoid gum bleeding
- Avoid high risk physical activities
- Maintain adequate nutrition, especially vitamin B12 and folate
- Limit alcohol intake
Regular medication review is important to avoid drugs that increase bleeding risk unless clearly indicated.

Conclusion
Low platelet count in elderly patients often signals an underlying condition or treatment effect. Some cases remain stable, but others carry significant bleeding risk. Early assessment allows timely intervention and reduces complications. Professional evaluation should not be delayed when thrombocytopenia is detected.
